For decades, we’ve fought cancer with the “Big Three”: surgery, chemo, and radiation. It’s often been a brutal trade-off — to kill the cancer, you had to damage the patient. But the physics of medicine is changing.
A new treatment called histotripsy is offering patients with inoperable liver tumors a better way: destroying the tumor without a single incision. By using focused sound waves, doctors can now break tumors apart while leaving nearby healthy tissue intact. For those who can’t go under the knife, this is more than just cool tech, it’s a literal lifesaver.
Physics vs Cancer
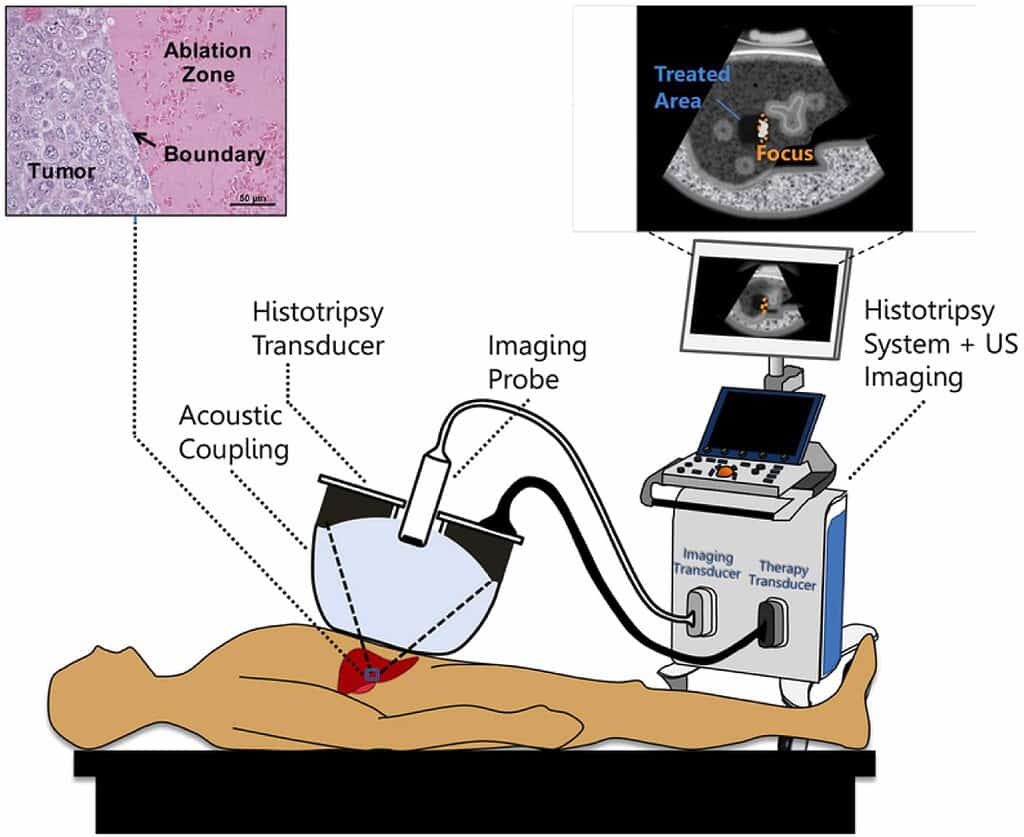
At its core, histotripsy is a masterclass in mechanical engineering. The name itself comes from the Greek for tissue breakdown, and it works exactly like that. The system focuses high-intensity sound waves into a tiny, precise point.
When these sound waves hit the target, they create a phenomenon called cavitation. In essence, the machine applies intense negative pressure to the fluid within the tumor, forcing microscopic bubbles to form and then violently collapse in a fraction of a second. This rapid-fire collapse creates a type of mechanical liquefaction, turning the tumor into a slurry of cellular debris that the body naturally clears out over the following weeks.
What makes this even more interesting is that it doesn’t use heat at all. Other methods (like microwave ablation, for instance) rely on heat to cook the cancer cells. But heat is messy and travels through the body. If a tumor sits too close to a major blood vessel or a bile duct, the heat can scar or destroy those vital structures. Histotripsy, however, is purely mechanical, sparing the collagen-rich walls of blood vessels and nerves while obliterating the softer cancer cells.
A recent study by Mustaqueem Pallumeera from Ohio State University acknowledged the promise of this new technique, noting that it “allows doctors to precisely target tumors while protecting nearby healthy structures through real-time image guidance.”
How Effective Is It?
For now, histotripsy has shown the most promise in treating liver cancer. The #HOPE4LIVER trial recently reported a staggering 95.5% efficacy rate in treating liver carcinoma and liver metastases using histotripsy. Within one to two months, the liquified tumor zones are often absorbed, leaving behind minimal scarring.
Because the method is new, there aren’t that many completed trials. However, the researchers note that there are strong positive early clinical signals in kidney tumors, while pancreatic and brain cancer data are still mostly preclinical or early-stage.
If liquefying a tumor wasn’t enough, histotripsy might have a second, even more potent effect: it could act as a vaccine against the patient’s own cancer.
The treatment can release tumor debris and inflammatory signals that may help trigger innate and adaptive immune responses, raising the possibility that mechanical ablation could work alongside immunotherapy. It even points to early evidence of systemic immune effects, though that remains an emerging area rather than settled fact.
Basically, when radiation or heat kills a cell, it often leaves a charred, unrecognizable mess. But when histotripsy’s bubbles shred a tumor, they release intact proteins and cellular “tags” called Damage-Associated Molecular Patterns, or DAMPs. These DAMPs act like a flare gun for the immune system.
Coming Soon or Decades Away?
Histotripsy is already here for some liver tumors, which makes it more than a futuristic concept. The US FDA cleared the first commercial histotripsy system for liver treatments in October 2023. Patients are being treated now, and the early results are strong enough to move the technology out of the lab and into carefully selected real-world care.
But for non-liver cancers, the timeline is murkier. Kidney tumors look like one of the next serious contenders, while pancreatic and brain applications still seem stuck in the harder phase: promising science, limited human evidence, and a lot of unanswered questions. The biggest hurdle is not whether sound waves can destroy tissue (they can) but whether doctors can do it reliably, safely, and better than existing options across very different organs.
Ultimately, the hold-up comes from a lack of large-scale, randomized trials to prove that patients actually live longer and stay cancer free with this type of treatment. The more support this type of research gets, the faster we can expect this type of surgery to become mainstream.
So, histotripsy does not look decades away. It looks like a technology in the awkward, fascinating middle stage: clinically real in one area, experimentally ambitious in others, and still waiting for the kind of long-term data that turns excitement into standard care. Our arsenal against cancer just got a shiny new weapon.
The study was published in PubMed.
This story originally appeared on ZME Science. Want to get smarter every day? Subscribe to our newsletter and stay ahead with the latest science news.